References
1. Meng NH, Lo SF, Chou LW, Yang PY, Chang CH, Chou EC. Incomplete bladder emptying in patients with stroke: Is detrusor external sphincter dyssynergia a potential cause? Archives of physical medicine and rehabilitation 2010;91:1105–1109.
2. Park DS, Choi DY, Lee JD, Kim YS, Nam SS, Lee SH. The acupuncture and moxibustion medicine Seoul: Jipmoondang; 2012. p. 479.
3. Kim TG, Chun MH, Chang MC, Yang S. Outcomes of drug-resistant urinary retention in patients in the early stage of stroke. Annals of rehabilitation medicine 2015;39:262–267.
4. Yu KW, Lin CL, Hung CC, Chou EC, Hsieh YL, Li TM, et al. Effects of electroacupuncture on recent stroke inpatients with incomplete bladder emptying: A preliminary study. Clinical interventions in aging 2012;7:469–474.
5. Curtis LA, Dolan TS, Cespedes RD. Acute urinary retention and urinary incontinence. Emergency medicine clinics of North America 2001;19:591–619.
6. Kim Y, Han T, Jung H, Chun M, Lee J, Kim D, et al. Clinical practice guideline for stroke rehabilitation in korea. Brain and NeuroRehabilitation 2009;2:1–38.
7. Lee M, Lee J, Choi T, Choi J, Jeon J. Preferred reporting items for development of clinical practice guideline in korean medicine Elsevier Korea: YJ Lee; 2015.
8. Lee MS. Preferred reporting items for development of clinicla practice guidline in korean medicine(pride-cpg-km) Daejeon: Korea Institute of Oriental Medicine; 2013. p. 118.
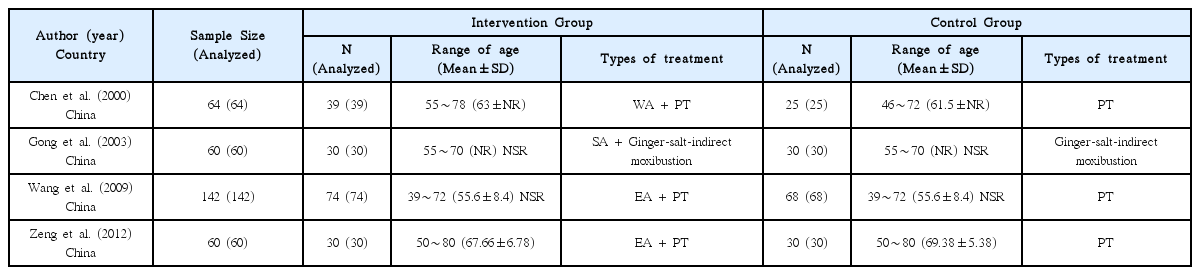
9. Chen S, Chen H, Yu S, LW D. Therapeutic effect of warm acupuncture for treating post-stroke urinary retention. Modern Journal of Integrated Traditional Chinese and Western Medicine 2000;9(6):530–531.
10. Gong Y. Treatment of post-stroke uriary retention with scalp acupuncture and ginger-partioned moxibustion. Zhejiang Jornal of Integrated Traditional Chinese and Western Medicine 2003;13(8):511.
11. Wang Z, Yang B. Clinical observation of effect of electro-acupuncture with physical bladder traning for post-stroke urinary retention. Journal of Mordern Urology 2009;14(2):121–122.
12. Zeng C, Zhou E. Clinical efficacy of electroacupuncture combined with bladder training in the treatment of post-stroke neurogenic bladder. Journal of Shandong University of Traditional Chinese Medicine 2012;36(6):513–515.
13. Park BW, Yoon JM, Moon BS. Review of clinical research on acupuncture treatment of voiding difficulty in stroke patients. J. Int. Korean Med 2015;36:153–164.
14. McGee MJ, Grill WM. Selective co-stimulation of pudendal afferents enhances bladder activation and improves voiding efficiency. Neurourology and urodynamics 2014;33:1272–1278.
15. Liu Y, Liu L, Wang X. Electroacupuncture at points baliao and huiyang (bl35) for post-stroke detrusor overactivity. Neural Regen Res 2013;8:1663–1672.
doi: 1610.3969/j.issn.1673-5374.2013.1618.1004.
16. Wang H, Deng D, Huang X. Clinical observation of 43 cases of post-stroke urinary incontinence treated by electro-acupuncture and pelvic floor muscle training. Journal of Qilu Nursing 2011;17(12):12–13.
17. Zhang Q, Cui Q, Song B. 50 cases of post-stroke urinary incontinence treated by electro-acupuncture and pelvic floor muscle exercise. Chinese Journal of Traditional Medical Science and Technology 2012;19(1):83–84.
18. Zhu Z. Clinical observation on 39 cases of urinary incontinence after stroke treated by acupuncture. Chinese journal of practical nervous diseases 2012;15(3):75–76.
19. Chu J, Bao Y, Zou C, Zhao H, Gong Y, Wang C. Clinical observation of electric acupuncture in treatment of non - inhibitory neurogenic bladder. Chinese Archives of Traditional Chinese Medicine 2012;30(10):2293–2294.
20. Feng X, Bai J. Clinical observation of electroacupuncture in the treatment of urinary incontinence after stroke. Guangming Journal of Chinese Medicine 2011;26(2):321–322.
21. Wu HM, Tang JL, Lin XP, Lau JTF, Leung PC, Woo J, et al. Acupuncture for stroke rehabilitation. Cochrane Database of Systematic Reviews 2006;:CD004131.
22. Li L, Zhang H, Meng SQ, Qian HZ. An updated meta-analysis of the efficacy and safety of acupuncture treatment for cerebral infarction. PloS one 2014;9:e114057.
23. Shen PF, Kong L, Ni LW, Guo HL, Yang S, Zhang LL, et al. Acupuncture intervention in ischemic stroke: A randomized controlled prospective study. The American journal of Chinese medicine 2012;40:685–693.
24. Huang F, Liu Y, Yao GX, Zhou FX, Wang XY. Clinical observations on treatment of ischemic stroke with acupuncture at back-shu points. Shanghai J Acupunct Moxibust 2008;10:4–7.
25. Schuler MS, Durdak C, Hol NM, Klink A, Hauer KA, Oster P, et al. Acupuncture treatment of geriatric patients with ischemic stroke: A randomized, double-controlled, single-blind study. Journal of the American Geriatrics Society 2005;53:549–550.