Introduction
Docetaxel, a type of taxanes, is widely used to treat breast cancer, non-small cell lung cancer, prostate cancer, gastric cancer, head and neck cancer. Some patients receiving docetaxel develop serious problems with fluid retention which is usually manifest as peripheral edema, pulmonary edema, or pleural effusions1).
Bangkihwangki-tang (“fangjihuangqi-tang” in traditional Chinese medicine; “boiogito” in Kampo medicine), one of representative prescriptions for edema in traditional Korean medicine, is first introduced in 『Synopsis of Golden Chamber』, a classic clinical book of traditional Chinese medicine written by Zhang Zhongjing at the end of the Eastern Han Dynasty, and it has been used in Northeast Asia over thousands years to treat several symptoms including edema, obesity, and arthritis. In these days, many investigators conducted research about BHT and reported various effects on edema2–4), obesity5), rheumatic arthritis6), osteoarthritis6), and urinary tract dysfunction7), etc.
This report presents the case of a patient with advanced gastric cancer that exhibited definite improvement on severe DIFR after treatment with herbal decoction, BHT.
Case Report
A 54-year-old male patient with advanced gastric cancer with multiple bone metastases was referred with pain, scleroderma, and edema over the both lower legs since two months ago. He was diagnosed with advanced gastric cancer, and then he received total gastrectomy followed by chemotherapy with capecitabine/oxaliplatin (XELOX), leucovorin/fluouracil/irinotecan (FOLFIRI) regimens and had several times of radiotherapies to metastatic sites. After disease progression, he subsequently received third line chemotherapy with docetaxel with total cumulative dose of 1230 mg/m2. Although docetaxel showed some efficacy to the patient, after four months of receiving docetaxel chemotherapy at cumulative dose of 930 mg/m2, problem of edema at the lower extremities accompanied with pain, scleroderma, and hypoesthesia, gradually deteriorated. Moreover, diuretics could not resolve the edema but caused moderate to severe adverse events such as nausea and vomiting. Furthermore, increased amount of pleural and pericardial effusion was detected by chest x-ray and chest computed tomography (CT) images. As a result, these adverse events made him change the chemotherapy regimen from docetaxel to paclitaxel. Also, his ambulation was possible only with help of wheelchair due to remarkable limitation caused by pain and edema at his lower extremities to move. From his first visit to our clinic, he was treated with herbal decoction BHT, widely used for edema in traditional Korean medicine and has shown hydrostatic modulating effect in several studies.
Treatment and Progress
At first visit to our hospital, he was unable to walk and showed poor performance status according to Eastern Cooperative Oncology Group Performance Status (ECOG PS) 3, due to grade 3 edema and grade 3 pain according to National Cancer Institute Common Terminology Criteria for Adverse Events (NCI-CTCAE) at his lower legs. The edema caused scleroderma, severe pain, and grade 2 hypoesthesia according to NCI-CTCAE.
The modified BHT (Table 1) was prescribed according to traditional Korean medicine theory to treat edema, and Aconiti Lateralis Preparata Radix was added to cope with feeling of cold at distal extremities. Herbal decoction was administered as liquid form three times a day. In addition, to promote circulation and preservation of Qi, non-herbal therapies including acupuncture (LI4, LI11 and SI3, bilaterally), moxibustion (CV4 and CV12), and cupping (Bladder Meridian alongside of the vertebral column, bilaterally) were routinely applied to the patient once a day.
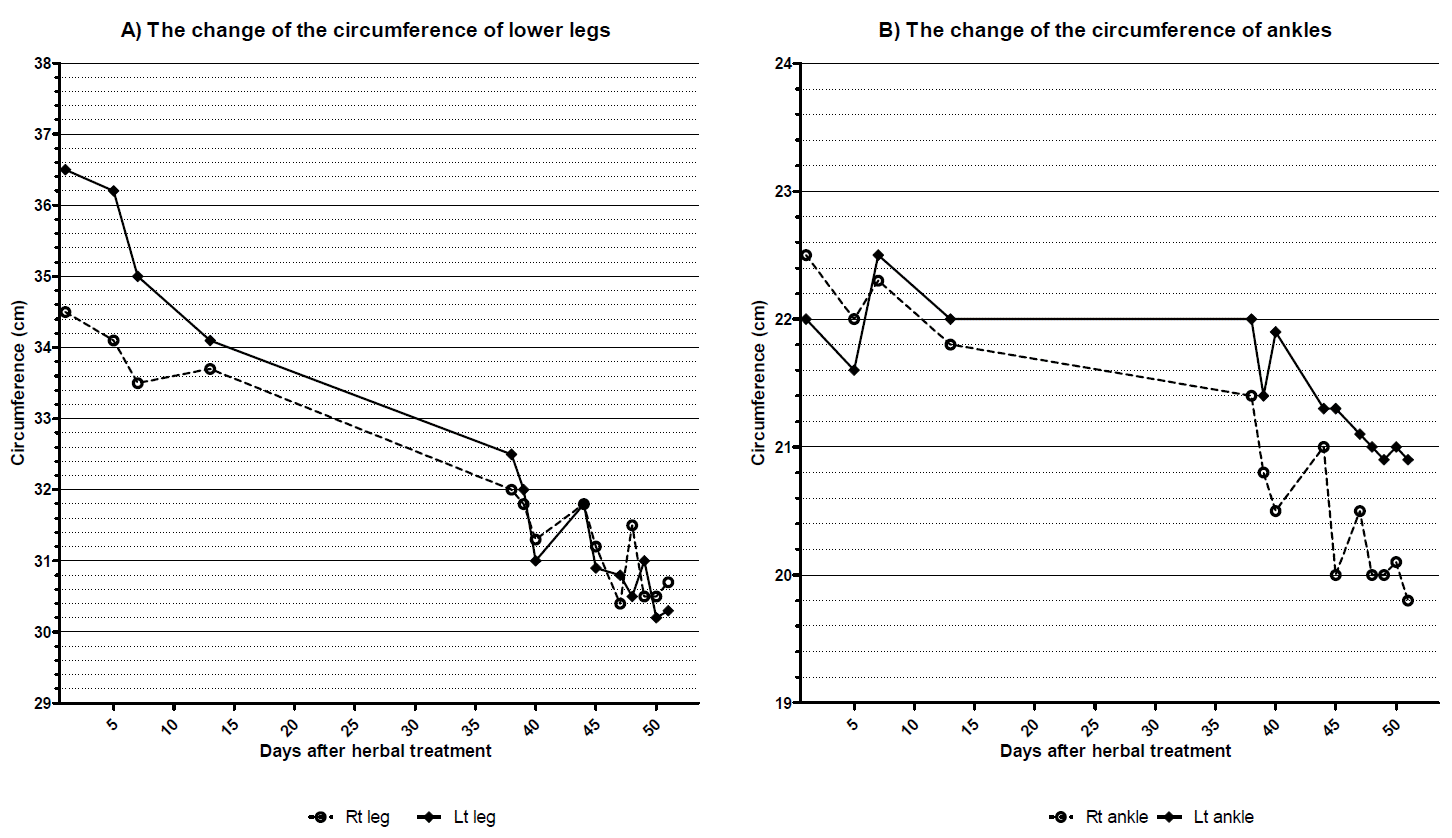
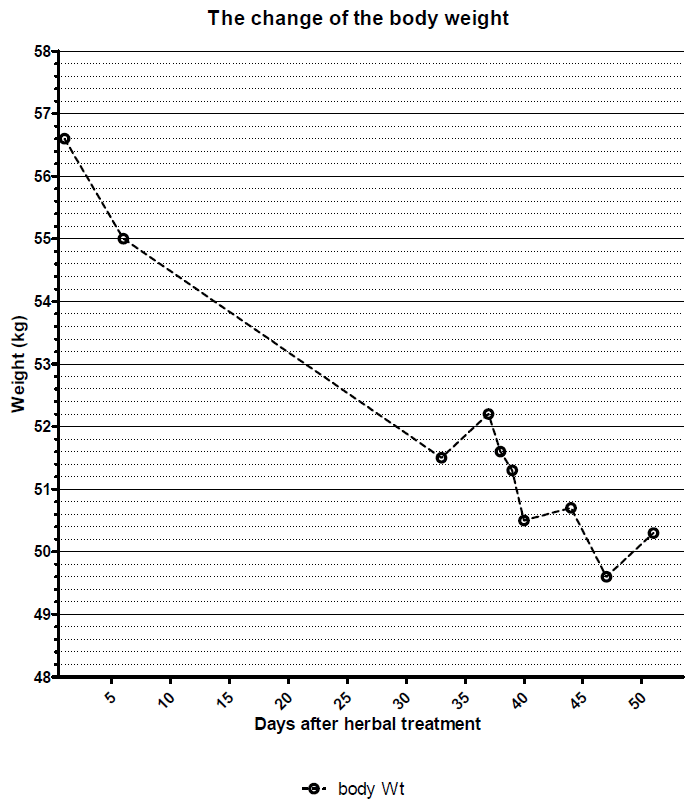
After the treatment, the edema had been gradually alleviated without fluctuation of urine volume or influence on electrolyte. Consequently the edema disappeared, and other symptoms such as pain, scleroderma, and hypoesthesia also improved. The improvement of edema was measured by change of circumference of legs and body weight (Figure 1, 2).
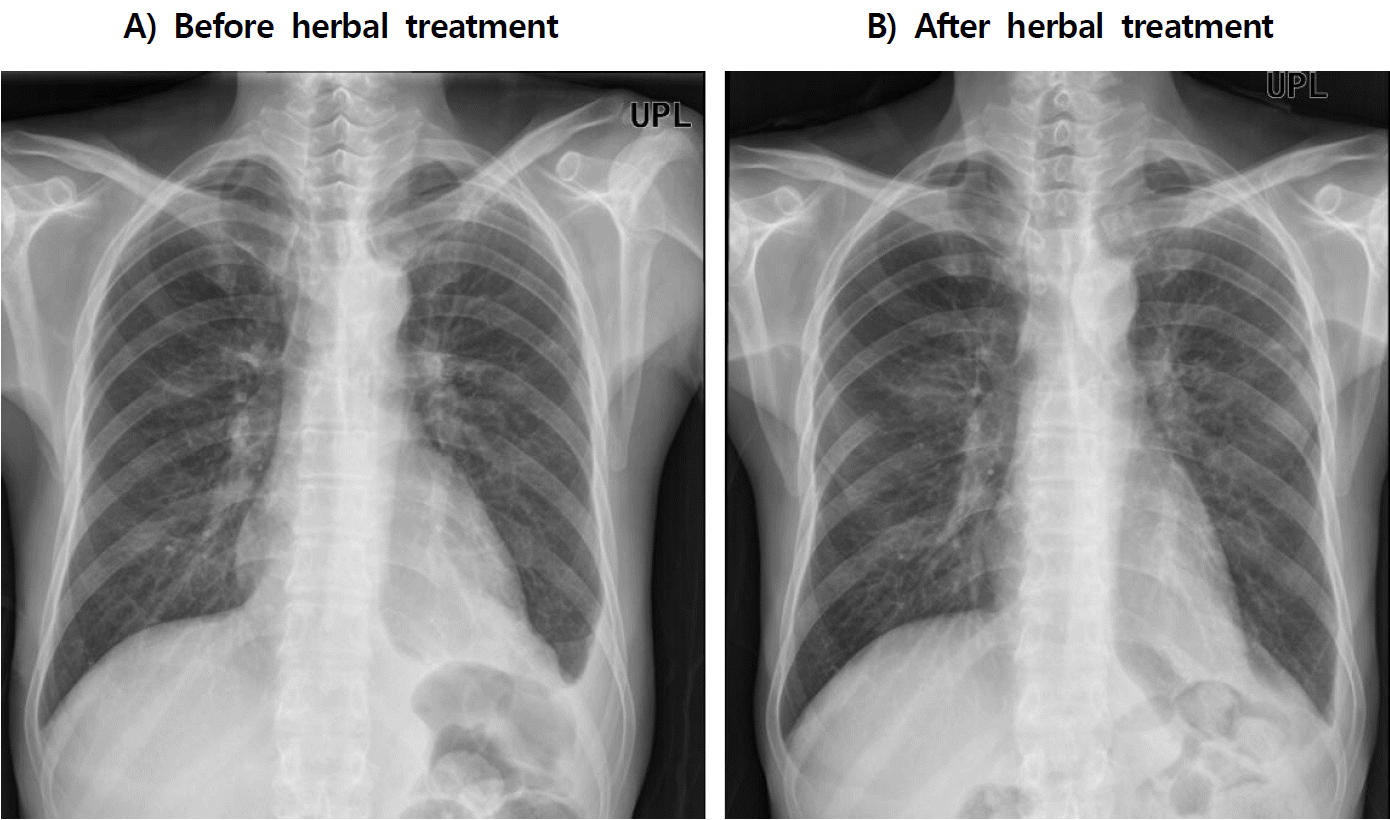
As the symptoms relived, he recovered from bedridden state and could able to walk on foot by himself about 165 meters at a time and the pleural and pericardial effusions has been decreased on radiographic images (Figure 3). Therefore, he was able to receive rehabilitation program to support walking motion and showed improvement in ECOG PS, from 3 to 2.
While he continued receiving paclitaxel chemotherapy, BHT was additionally administered and, it took him three months to resolve all of the symptoms of the patient without additional use of diuretics or glucocorticoids except chemotherapy premedication. Also, BHT-related adverse effects were not observed. And, his albumin levels were remained stable (approximately 3.5 g/dL).
Discussion
The occurrence of DIFR related to the total dose of docetaxel was administered; it appears at an average cumulative dose of 400 mg/m2 without glucocorticoid premedication. However, in phase II clinical trials, glucocorticoid premedication increased the median cumulative dose to onset of moderate or severe fluid retention from 490 mg/m2 to 790 mg/m2 while reduced the incidence of severe fluid retention from 20 to 6 % and the discontinuation of treatment from 32 to 3 %8,9). Most DIFR is reversible after withdrawal of docetaxel (median time to resolution between 16 and 20 weeks), except severe cases in 5 to 6 % of patients10).
The usual initial symptom is peripheral edema and weight gain, and early treatment with diuretics contributes to limiting the severity of DIFR. But continuation of docetaxel chemotherapy with un-controlled fluid retention may progress to pleural and/or pericardial effusions, pulmonary edema, and ascites which may lead to withdrawal of treatment. At first, the appearance of edema was soft pitting pattern and localized at lower part of the body, but it became hard and extended to the whole body disturbing movement of joint after lymphatic involvement11).
Although the underlying mechanism of DIFR is not fully understood, some studies suggest the underlying rationale about pathophysiology of DIFR. In early stage, excessive trans-capillary filtration of proteins (capillary protein leakage) and the primary toxic effects on the capillary endothelium result in congestion of the interstitial space by proteins and waters. Later, mainly after the fifth cycle, insufficiency in lymphatic drainage occurred, inducing clinically obvious fluid retention11,12).
Although there was no study about BHT on DIFR, hydrostatic modulating effects of BHT have been reported to control body fluid imbalances in patients suffering from edema. In several in vivo studies, “Ohnishi et al.” reported moderate diuretic effects of BHT in hypervolemic mice but not in euvolemic mice2). “Kim et al.” reported that BHT significantly increases urine output via up regulation of renal hemodynamics and down regulation of sodium reabsorption in rabbit3). In clinical study, “Milan et al.” reported that administration of BHT in patients with chronic heart failure and renal insufficiency significantly ameliorated renal function, improved estimated glomerular filtration rate4). Considering these results, we think BHT as the main component in treat DIFR through hydrostatic modulating effects. Other therapies such as acupuncture, moxibustion, and cupping may be contribute to these hydrostatic modulating effects, but there is not enough evidence about their direct and/or indirect effect on DIFR for now.
In this report, the patient received third line chemotherapy with docetaxel along with prophylactic dexamethasone, a member of glucocorticoid class of steroid drugs. After cumulative dose over 930 mg/m2, he shows significant clinical manifestation of severe fluid retention, grade 3 according to NCI-CTCAE. Moreover, furosemide and spironolactone, prescribed diuretics for the fluid retention, were not effective, but rather caused moderate to severe nausea and vomiting. As prophylactic steroid and diuretics therapies became unresponsiveness, there is no other way but to stop docetaxel chemotherapy and use other chemotherapy regimen. So, the patient came to our clinic to manage DIFR through traditional Korean medicine.
Since the start of treatment with herbal decoction, BHT, the patient showed subjective improvement such as relief of pain and decrease of scleroderma at his legs. The alleviation of fluid retention was measured with objective methods such as, circumferences around legs, body weight, and radiologic images over a period of time. The recovery time of this patient was 14.5 weeks which is shorter than previously reported median time to recovery from DIFR (median 16–20 weeks10)). Until now, even though the symptoms almost disappeared, no herbal treatment related adverse event has been reported; he is still continuing the rest of chemotherapy cycles without any severe problems. The immediate improvement of DIFR after applying the herbal treatment and the shortage in the recovery period regarding the severity of the initial symptoms strongly prove the therapeutic potential of BHT.
However, there are several limitations to claim the effect of BHT on DIFR. First, even though the positive reaction of herbal treatments certain, the possibility of natural resolution of DIFR as a result of natural process after withdrawal of docetaxel cannot be ruled out completely. Unfortunately, there is lack of data about natural resolution period after withdrawal of docetaxel in advanced gastric cancer patients. Other study in metastatic breast cancer patient reported median resolution time 16–20 weeks from withdrawal of docetaxel10). Second, the fact that the result was observed only in one patient makes it hard to generalize efficacy of BHT on DIFR.
Summary
In conclusion, this is the first case report about therapeutic potential of herbal medicine, BHT on DIFR. This result suggests BHT as an alternative option to manage the patients suffering from adverse events of docetaxel chemotherapy. Further clinical experiences and researches on its mechanism will be needed to elucidate the efficacy of BHT on DIFR.