Introduction
Samul-tang (SMT, Si-Wu-tang in Chinese; Shimotsu-to in Japanese) is traditional herbal formula composed of 4 different crude herbs; Angelicae Gigantis Radix, Cnidii Rhizoma, Rehmanniae Radix Preparata and Paeoniae Radix. SMT has been used for treatment of gynecological diseases such as postmenopausal syndrome, menstrual irregularity, infertility and toxemias of pregnancy in traditional medicine (TM). To date, many researchers have reported its various pharmacological effects including anti-inflammation1)2), anti-neural damage3) hematopoiesis4,5). Despite various efficacy of SMT, few scientific works have explored the safety of this herbal medicine.
Toxicology is a subject to study safety and the adverse effects of chemicals or physical agents6). Recently, drug toxicology studies have not been applied only to single compounds but to crude extracts as well as cocktail drugs like herbal formulas. Safety evaluation of the drugs includes acute, subacute, subchronic, chronic and genetic toxicity tests. Among them, acute toxicity refers to the adverse effects occurring after oral administration of single dose or multiple dose of substance given within 24 hours7). The purposes of acute toxicity tests are to obtain biochemical and pathological changes, which provide information for sub-acute toxicity tests. Thus, acute toxicity studies in animals are an essential step for single-dose-administered pharmaceuticals that are intended for human use.
We here investigated the acute toxicity of SMT in Sprague Dawley (SD) rats, to evaluate its safety and toxicity profiles. Due to the results of our toxicity study, we have established scientific evidence that SMT is harmless.
Materials and Methods
1. Preparation of SMT
A decoction of SMT was prepared as previously described8). Briefly, a mixture of four ground herbal medicines (Table 1) was boiled in distilled water at 100°C for 2 h. The extract was condensed using freeze-drying (yield: 33.3%), dissolved in distilled water and mixed well. The solution was filtered through a SmartPor GHP syringe filter (0.2 μm pore size, Woongki Science, Seoul, Korea).
2. Animals and maintenance
Twenty specific pathogen-free 5-week-old Sprague Dawley (SD) rats of each sex were obtained from Orient Bio Co. (Seoul, Korea). All the rats were housed at a constant temperature (23±3°C) and humidity (50±10%) with a 12 h light/12 h dark cycle, 1020 air changes per hour and a light intensity of 150–300 Lux. The animals were kept in stainless steel cages at ≤2~3 animals per cage for the observation period. They were fed a rodent chow diet (PMI Nutrition International, Shoreview, MN, USA) and sterilized tap water ad libitum. This study was performed in the Korea Institute of Toxicology (earned AAALAC International accreditation in 1998) under the Good Laboratory Practice Regulations (GLPR) for Nonclinical Laboratory studies9). The present study was monitored by the Organization for Economic Cooperation and Development (OECD) and the Korea Food and Drug Administration (KFDA).
3. Experimental groups and treatments
To determine a proper dosage of SMT for acute toxicity tests, we performed a test of a single oral administration of SMT at a dose level of 1250, 2500 or 5000 mg/kg/day. SMT did not induce any toxic effect at any of these doses. Based on these results, the highest dose level of 5000 mg/kg/day was chosen for the acute toxicity study. Healthy animals were divided into four groups (n = 5 per group) using Path/Tox System (Version 4.2.2, Xybion Medical System Corporation, Morris Plains, NJ, USA). Because oral administration is the clinically intended route for SMT, it was administered by oral gavage in the present study. Prior to each daily administration, SMT was suspended in distilled water. The daily application volume (10 mL/kg body weight) of SMT was calculated based on the recorded body weights of individual animals. The vehicle groups received an equal volume of distilled water.
4. Clinical signs and mortality
Clinical signs and mortality were recorded continuously until 6 h after treatment and then once a day from the following day throughout the study period.
5. Body weights
Body weights were measured before SMT treatment (day 1) and on days 2, 4, 8 and 15 after treatment.
6. Gross findings
All the animals were anesthetized by carbon dioxide and then sacrificed by exsanguination from aorta at the end of the experiments. Gross examinations were observed with naked eyes to all vital and tissues.
7. Statistical analyses
Body weights were presented as mean ± standard deviation (SD). Statistical analyses were performed F-test using the Path/Tox System 4.2.2. Differences from the normal control were regarded as significant if p < 0.05. Statistical analyses for calculating the median lethal dose (LD50) value were not performed because no mortality was observed.
Results
2. Body weights
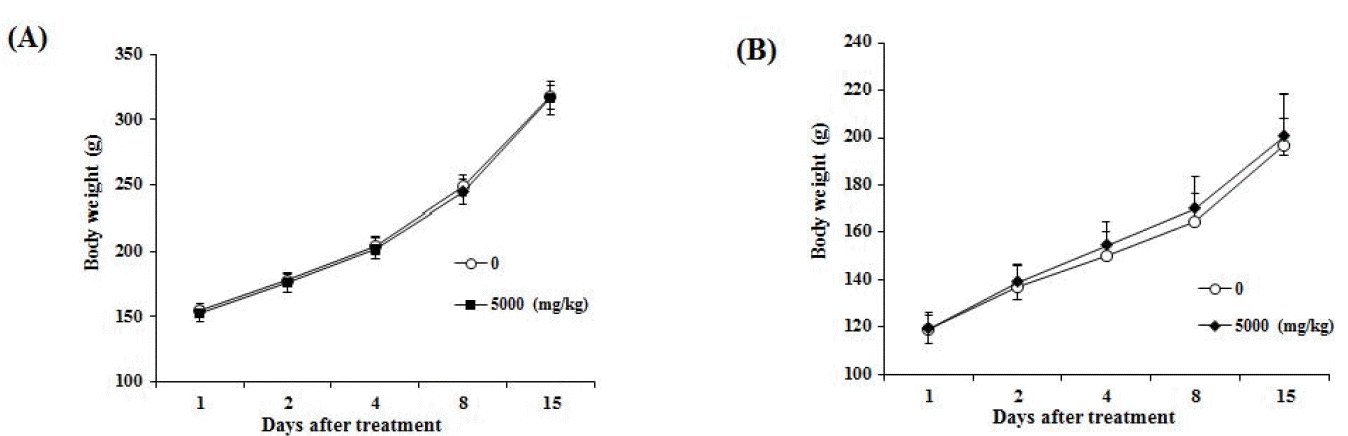
In both sexes, there was no adverse effect in the SMT-administered group compared with the vehicle control group (Fig. 1).
3. Gross findings
No treatment-related gross pathological changes in internal organs including lung, heart, thymus, stomach, liver, adrenal, spleen were observed in any groups (Table 4).
Discussion
Traditional herbal medicines including herbal formulas and medicinal herbs have been used for centuries in Korea, China and Japan. In general, herbal formulas are made up of several different medicinal herbs that contain various active compounds. Many researchers have worked to establish scientific evidence of the efficacies of herbs and herbal prescriptions10),11,12). However, recent studies have led to increasing concern about the safety and toxicity of herbal prescriptions13,14). Contamination of herbs with metals and dosage miscalculation can lead to an increased risk of side effects10). Thus, control of herb quality and evaluation of herb toxicity are urgently required to provide essential information for their clinical use.
Several previous studies indicated safety of SMT using animal models. Ma et al. reported that SMT didn’t have any toxic effect on ICR mouse at the doses of up to 5000 mg/kg15). Yu et al. also reported that there was no adverse effect on SD rats at a dose of 1500 mg/kg during repeated administration of SMT for 28 days16). These studies suggested that SMT could be a safe prescription for humans. However, these studies were not performed under GLP standards. GLP refers to a system of quality management controls for process and condition in non-clinical laboratory studies9). The toxicity evaluation of a chemical mixture is necessary to guarantee its safety, therefore toxicity tests must be conducted in compliance with GLP guidelines to ensure reliability. Our study was conducted under GLP guidelines and confirmed the safety in male and female SD rats fed a single dose (5000 mg/kg) of SMT by GLP practices.
Consistent with previous results, the present study using SD rats showed no abnormal changes in mortality, body weight or clinical signs in rats of either sex (Tables 2–4 and Fig. 3). These results imply that SMT did not induce any adverse effects at an oral dose of up to 5000 mg/kg/day. Thus, the LD50 was considered to be greater than 5000 mg/kg regardless of sex. Moreover, a single dose of SMT in humans is about 18.76 g dried herb, which is equivalent to 6.25 g of SMT extract (yield = 33.3%). Considering that the average weight for an adult is 60 kg, this dose for human is equal to 104.1 mg of SMT extract/kg. This dosage is 48-fold lower than the LD50 of SMT.
In conclusion, we confirmed SMT shows no toxicity in SD rats after treatment with a single oral dosage. Since traditional herbal formulas are usually taken for a longer period, further studies will be needed to establish the safety information on SMT including repeated oral toxicity and genotoxicity.