Introduction
Hepatitis A is a kind of viral hepatitis, with the incidence rate of approximately 1000 to 10,000 cases annually in Korea and 4000 to 30,000 cases in USA.1,2) Hepatitis A virus (HAV) belongs to the family picornaviridae and the genus hepatovirus, and is a non-enveloped RNA virus with the diameter of 27 nm.3,4) HAV viral transmission occurs in a fecal-oral fashion; therefore, hygiene and socio-economic status play important role in hepatitis A pathology.5)
After infection, HAV lies dormant for approximately 25 days, and infectivity is the strongest in this stage. Then, the subsequent hepatic cell damage causes elevation of serum liver enzymes and influenza-like symptoms such as fatigue, weakness, anorexia, nausea, vomiting, abdominal pain, and fever. This is followed by elevated bilirubin stage, causing jaundice.6) Hepatitis A is highly contagious, but does not become chronic, and symptomatic treatments, such as resting and providing sufficient nutrition, are enough due to spontaneous cure within 6 months.7) However, about 15 % of hepatitis A cases have a prolonged clinical stage of over 6 months, and 20 % of hepatitis A cases relapse within 2 to 3 months.8) Although for a small percentage, hepatitis A can cause complications, such as acute liver failure, renal failure, interstitial nephritis, pancreatitis, red blood cell aplasia, and so on. Fulminant hepatitis occurs in 0.14~0.35 % of hepatitis A cases, which may require liver transplantation.9) Recently, reports of poor prognosis of hepatitis A, including such complications as liver transplantation, and death have been steadily increasing in the developed countries including Korea.10,11) Furthermore, many cases of hepatitis A could be misdiagnosed as a common cold, which leads to administration with antipyretic analgesic including acetaminophen, most of which have to be avoided.12)
Korean medicine (KM) describes hepatitis A as jaundice, a typical symptom of hepatitis A. In fact, approximately 70 % of hepatitis A cases present jaundice. Hepatitis A has been well controlled in KM clinics from the ancient period; however, to the recent ban on chemical/immunological diagnostic tools, it has become a rare disease treated by Oriental doctors.
Therefore, this case study presents severe hepatitis A in a 20’s male in the 2019 outbreak of hepatitis A in Chungcheong-do province, Korea will arouse awareness of the misdiagnosis of hepatitis A and provide therapeutically useful information in Korean Medicine-based treatments.
Report of the case
1. Patient and diagnosis
A 25-year-old male felt sudden severe fatigue and pantalgia. He thought he had a cold and took over-the-counter medicine (Dexibuprofen 300 mg, Acetaminophen 320 mg) for two days. However, symptoms did not resolve, and when his urine became darker, the patient visited a KM hospital on Sep. 10th. 2019. He did not remember personal or family history of liver disease. He denied traveling, eating contaminated food or water, and consuming alcohol, energy drinks, or illicit drugs within the last two months. On physical examination, mild jaundice of the sclera was observed, and there was a mild tenderness in the epigastric point. The tongue was red without fur, and the pulse was floating. His symptom differentiation was the “Accumulation of damp heat(濕熱蘊結)”. The initial serum liver enzymes were more than 100 times higher than the normal range (AST 4,621 IU/L and ALT 2,763 IU/L). Total bilirubin (4.4 mg/dL), γ-GTP (227 IU/L), ALP (151 IU/L) and monocytes portion in CBC (21.0%) were also notably elevated. Anti-HAV IgM was elevated to 6.58 signal cutoff (S/Co), and other hepatitis virus tests were negative. There was no significant abnormal shadow on Abdomen X-ray. Based on these results, he was diagnosed as hepatitis A and hospitalized.
2. Treatment and course of symptoms
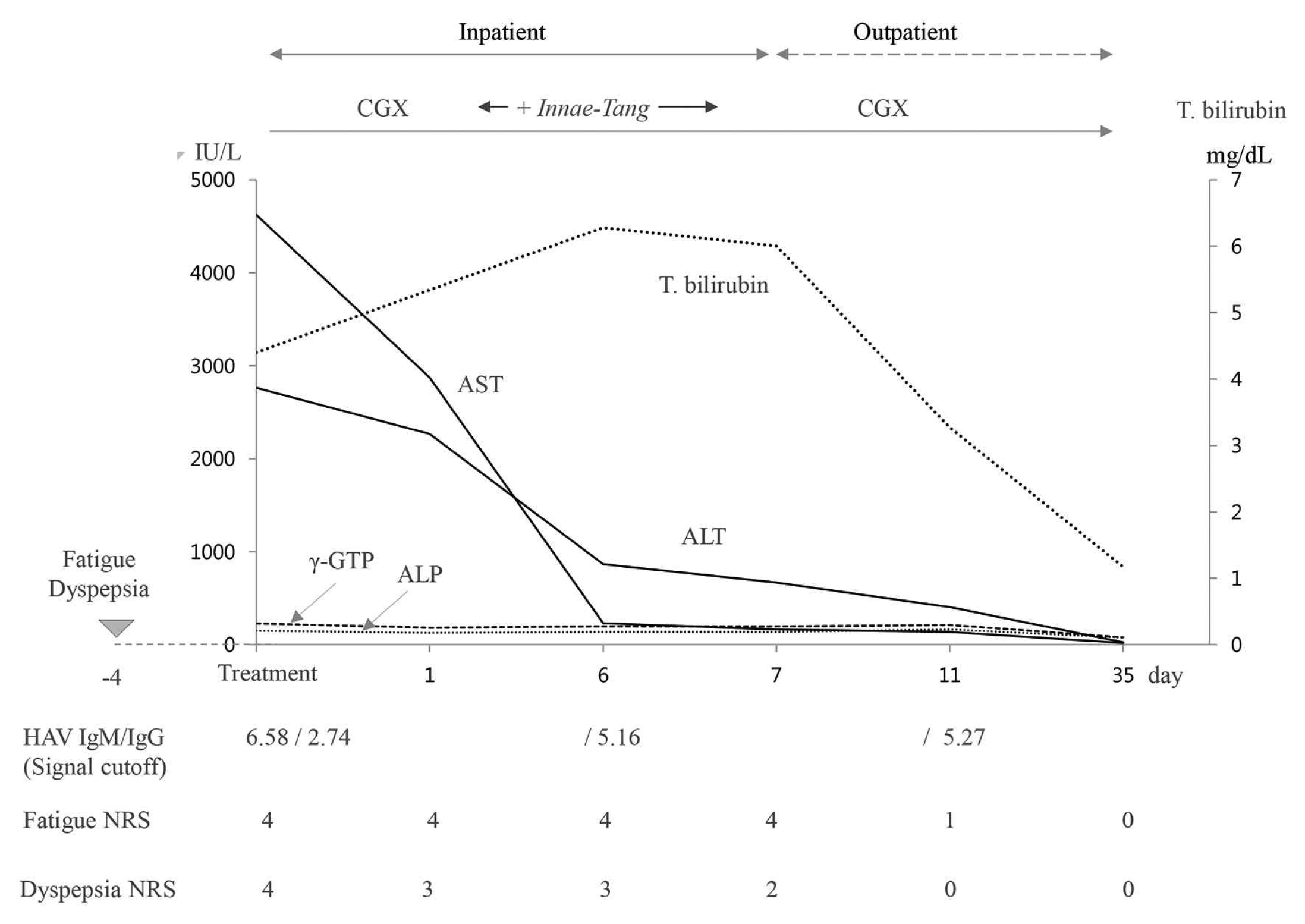
Based on the diagnosis of hepatitis A, two herbal drugs CGX and Innae-Tang (Table 1) were given to the patient, 3 times a day. Acupuncture was performed twice daily (morning and afternoon) mainly at LI4 (合谷), LR3 (太衝), PC6 (內關), SP4 (公孫) for 15 minutes at the depth of 10mm. To provide sufficient volume and nutrition, 1000 ml of dextrose 5 % mixed with a vitamin complex was supplied intravenously each day. Improvement of the symptoms was soon noted: fatigue on Day 4 and dyspepsia on Day 7. On Day 8, AST (163 IU/L), ALT (667 IU/L) was decreased, and the patient discharged on Sep. 18th. 2019. The subsequent blood tests showed the normalization of items including AST (20 IU/L), ALT (27 IU/L), and total bilirubin (1.17 mg/dL) on Day 35 (Figure 1).
Discussion and Conclusion
HAV is usually an asymptomatic infection in young children, but its clinical symptoms become more severe in adults.13) In recent years, hygiene in South Korea has dramatically improved, and seroprevalence of HAV has changed.14) In the young adult group, HAV seropositivity was over 80 % during the 1970s, but decreased to below 20 % in 2006.15) Accordingly, the high susceptibility to HAV in young adults increases the incidence rate of hepatitis A with a poor prognosis. Pandemics occurred in 2009 and 2019.16,17) In 2009, 15,231 people were diagnosed with hepatitis A in 2009; in 2019, this number reached 17,636.18,1)
The case reported in this study showed a severe liver injury, which required attention for the risk of a poor prognosis. In clinics, many doctors could misdiagnose hepatitis as a cold and usually prescribe non-steroidal anti-inflammatory drugs or acetaminophen. However, as these drugs can aggravate liver damage, these drugs should be avoided by patients with hepatitis A.19) Doctors should consider the possibility of an HAV infection in any case with complaints about digestive problems and cold-like symptoms, especially in the periods of hepatitis A pandemics in the region. Prior to presentation, the patient of our study took acetaminophen 640mg for 2 days. However, upon receiving CM treatment, the patient recovered within one week in terms of his subjective symptoms, and within 5 weeks in terms of the laboratory abnormalities. The slight abnormality of γ-GTP (81 IU/L) on Day 35 can be explained by the fact that this enzyme will take longer than other enzymes to improve to the normal range.20) The increased portion of monocytes in the CBC test might have resulted from the fact that HAV inhibits the differentiation of monocytes.21)
CGX is an hepato-therapeutic syrup composed of 13 herbs, and its pharmacological activities were proved in preclinical and clinical studies,22) while Innae-Tang (Artemisiae Capillaris Herba plus Raphani Semen (see Table 1) can eliminate dampness and removes X.23,24) Acupuncture points (LI4, LR3, PC6 SP4) were selected to facilitate digestion and help the Qi (氣) and blood circulation as recommended in a previous study.25) Regarding herbal drugs, there are many considerations for the hepatotoxic effects in the patients with hepatic inflammations and other disorders.26) However, there is evidence that the risk of herb-related hepatotoxicity is overestimated.27) As shown in this case report, the proper use of herbal drugs could be a better option in treatments of various liver disorders.28) In summary, the adequate level of hygiene and vaccination resulted in a very low incidence of hepatitis A; however, certain age groups (people in the 20s to 40s in South Korea) are risk groups for the HAV infection. Accordingly, doctors should consider the possibility of HAV infection when hepatitis A is pandemic, particularly in younger patients (aged in their 20s and 40s). In addition, KM-based treatments is an appropriated option for hepatitis A. The present case report provides meaningful insights for the prevention, management, and treatment of hepatitis A.